Latest News
Drivers urged to use caution as Kent road work begins Monday
Aly Morrissey
Jun 08, 2026
Routine road work is scheduled to begin on several roads Monday, June 8, in Kent.
Ruth Epstein
KENT – Drivers in Kent should use caution Monday, June 8, as routine road maintenance is scheduled to begin on several roads. Highway crews are preparing for annual chip-sealing projects, a process used to repair or extend the lifespan of paved roads.
The following roads are scheduled for treatment:
- Geer Mountain Road (from Ore Hill Road to Jennings Road)
- Ore Hill Road
- South Road
- Kenmont Road
- Bulls Bridge Road (from Route 7 to No. 160)
- Macedonia Brook Road
Town officials said the work is weather dependent and delays or rescheduling are possible. The work is expected to take between three and four days, weather permitting. Temporary speed limit reductions will be in effect because of loose stone on the roadway.
Drivers are urged to follow traffic directions, use caution in work zones and reduce their speed to avoid throwing loose stones into the windshields of passing vehicles.
Residents with questions may contact the Kent Selectman’s Office at 860-927-4628.
Keep ReadingShow less
Man drowns after kayak overturns in North Canaan pond
Aly Morrissey
Jun 06, 2026
A Lifestar helicopter prepares to land after a fatal drowning in North Canaan on Saturday, June 6.
John Coston
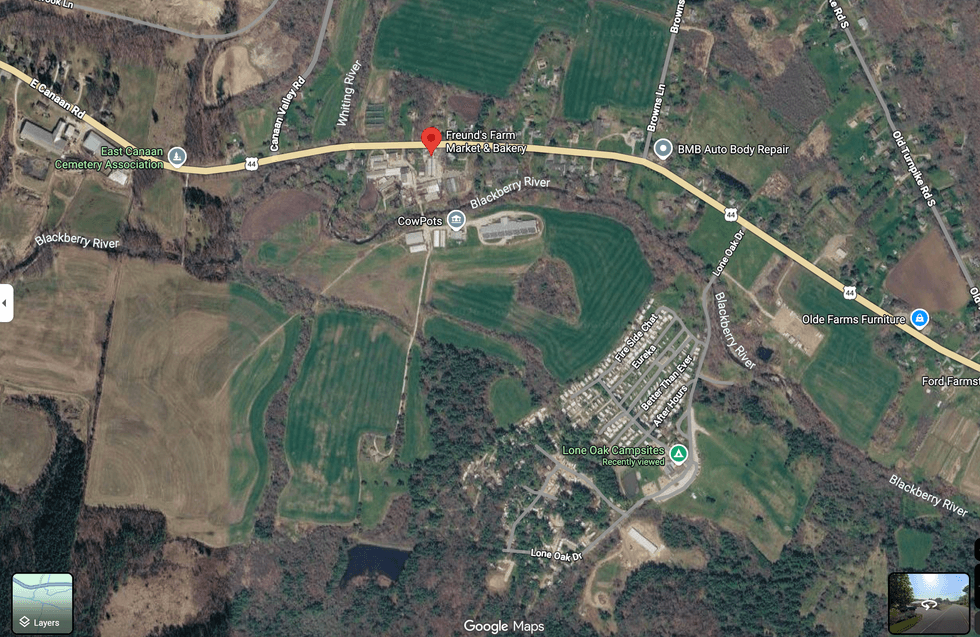
NORTH CANAAN – An adult man drowned Saturday afternoon, June 6, after a kayak overturned in a private pond behind Freund’s Farm Market and Bakery.
The man was the sole occupant of the kayak, according to officials. DEEP Environmental Conservation Police (EnCon) responded along with North Canaan emergency responders and Connecticut State Police Troop B.
The man was recovered from the pond, but life-saving efforts were unsuccessful. He was pronounced dead.
A Lifestar helicopter was seen landing in the area near the Lone Oak Campsites in East Canaan, though it did not land on the campground property, according to employee Jean Goodall. She said the helicopter was visible from the campground.
According to emergency dispatch records the man was pulled from the water just before 1:15 p.m.
DEEP Environmental Conservation Police are leading the investigation, which is ongoing.
Keep ReadingShow less
Yerger Johnstone
Lakeville Journal
Jun 03, 2026
SHARON — Yerger Johnstone, former managing director in the mergers and acquisitions department at Morgan Stanley and a decorated veteran of the Vietnam War, died on April 19, 2026, in Chelmsford, England. He was 86.
Born in Mobile, Alabama, on March 7, 1940, Mr. Johnstone was the son of architect Henry Inge Johnstone, architect, and Kathleen Yerger Johnstone, the noted nature writer and civic leader after whom Alabama’s state seashell, Johnstone’s Junonia, is named. He graduated from Murphy High School in Mobile in 1958, received his bachelor’s degree from the University of the South at Sewanee in 1962, and earned his M.B.A. from the University of Chicago Booth School of Business in 1964.
Following his M.B.A., he was commissioned through Officer Candidate School before serving in the United States Marine Corps from 1966 to 1968, rising from First Lieutenant to Captain. Stationed principally at Da Nang, Vietnam, he served as an intelligence officer and was awarded the Bronze Star with combat “V” for meritorious service.
Yerger married Eve Chamberlain, also of Mobile, Alabama in 1963 and they resided in North Carolina during this USMC training. Later moving to Brooklyn, New York, where his first child, Bartley, was born in 1968.
After his discharge, Mr. Johnstone joined Morgan Stanley, working in both Paris and New York City, where he became one of the firm’s first forty partners and served as deputy director of the Mergers and Acquisitions department under Robert Greenhill, at the very dawn of the M&A boom. He later worked in M&A at Blackstone and UBS Warburg Dillon Read. He also served on the boards of Hampshire College and Indian Mountain School at different times in his life.
Yerger was an accomplished sailor, having grown up on boating excursions for shell hunting with his parents in areas of Alabama and Florida, later on receiving certifications in sailing trips around Corsica while working in Paris. While working in banking in the late 1970’s and early 1980’s he spent evenings and weekends reading sailing training manuals, autobiographies of sailors and geographies of various archipelagos, further advancing his skills with a month of yacht chartering each summer in Greece.
Yerger first became enchanted with Litchfield County, when he and his second wife, Marguerite, found their dream weekend escape in Ellsworth in Sharon, Connecticut in the mid 1970’s. A one time builder of hot rod cars in his teens, he enjoyed spirited late night drives from NYC in a friends loaned Ferrari. In Ellsworth the newly weds and then young family (when his second daughter Katherine was born) enjoyed many weekends, hiking, bird watching, star gazing, cross country skiing, growing fresh herbs and gardening and barbecuing Yerger’s famous steaks for guests. Yerger enjoyed exploring the back roads of the area on his BMW motorcycle and the Housatonic River as an avid fly fisherman.
Upon leaving Morgan Stanley, he and his wife Marguerite whom he married in 1975, built the 67-foot ketch Asteroid in Aalsmeer, Holland. They conducted sea trials in Norway, Scotland, Ireland, & England before sailing her around the world, a near 6 year circumnavigation, passing via Suez and Panama canals, spending majority of the time in Pacific Ocean isles from Marquesas to Fiji, New Zealand (where his son Rule was born in 1986) and Micronesia. Encounters with storms, pirates, technical difficulties in remote islands and simply the rigors of daily yachting life were all met with courage, confidence and enthusiasm by Yerger. It became one of the defining adventures of his life.
Returning to America at the end of the sailing trip in 1990, the family settled in Falls Village, Connecticut, where they lived and built a house until Yerger was transferred to London, England
Yerger lived between Salisbury, Connecticut, and the UK for several years before permanently relocating to live between the Cotswolds in the UK and Tuscany in Italy with his third wife, Pamela. They enjoyed an active retirement with regular travels in Asia, New Zealand and Greece. In his final years, he was mainly in his homes in Italy and UK, with short trips in France, with his second daughter. In Trequanda, Italy he enjoyed cycling, feasting at home and throughout Tuscan villages with his and Pamela’s many friends, and soaking up the Tuscan sun. In his home village of Stebbing, UK, he headed the local pond fishing club and took short trips to London to hear his daughter Katherine sing in her many choirs.
Mr. Johnstone is survived by his wife, Pamela Johnstone; his daughters, Bartley Inge and Katherine Inge; his granddaughter, Evie Inge Scofield; his son, Rule; his former wife, Marguerite; his brother, Justice Douglas Inge Johnstone. He is predeceased by his first wife, Eve Chamberlain Purdy.
Cremation took place May 18, 2026, at Dunmow Crematorium, Blatches Farm, Stebbing CM 6 3AL England.
There will be a Requiem Mass said on June 7th, at St George’s Aubrey Walk, W8 7JG England.
Keep ReadingShow less

Want more of our stories on Google? Click here to make us a Preferred Source.
Richard R. Stover
Lakeville Journal
Jun 03, 2026
WEST CORNWALL — Richard R. Stover, 82, of West Cornwall, died peacefully at Noble Horizons on May 26, 2026.
Son of the late Robert and Leona (Heinbockel) Stover, Rick was born Feb. 6, 1944 in Edina, Minnesota. He attended the University of Pennsylvania where he majored in Economics and was a member of Sigma Alpha Epsilon fraternity.
After graduation, Rick began a long career as a financial and pharmaceutical analyst working at Mitchell Hutchins, Smith Barney, Alex Brown & Sons, Pfizer, and Arnold and S. Bleichroeder. He was then President and CEO of PeriCor Therapeutics, a bio tech company he founded in Manhattan.
Rick was an avid golfer and skier, and he liked nothing better than wrestling with the wilderness. After he and Marnell bought their home in West Cornwall, he enjoyed clearing brush, felling trees, and splitting logs. He was the proud owner of every tool and machine necessary for landscape maintenance.Rick was a parishioner at St. Bridget Church where he worked on the building and grounds committee and served as Chairman of the Finance Council.
Rick is survived by his wife Marnell (Bukovac) and his four daughters and their families; Shaw (Christofer) Ruder and Beckett, Elliot, and Hattie; Sara Stover (Chris Sherwin); Christian Stover (Jeffrey Knutsen); Anne (Andrew) Ruder and William, Charlie, and Sadie. He is also survived by his stepchildren and their families: Mary Brunelli (Christopher Edgar) and Alexander and Catherine; and Michael (Ellen) Brunelli.
Rick was preceded in death by his sister Barbara McCurdy.
A Mass of Christian burial was held at St. Bridget Church (St. Kateri Parish) 7 River Road, Cornwall Bridge, on Saturday, May 30, 2026 at 11:00. Burial followed at St. Bridget Cemetery.
Contributions in Rick’s name may be made to St. Kateri Parish (St. Bridget Church), PO Box 186, 90 Cobble Road, Kent, CT 06757.
The Kenny Funeral Home has care of arrangements.
Keep ReadingShow less
Floyd Irving Isham
Lakeville Journal
Jun 03, 2026
SHARON — Floyd Irving Isham Jr., 87, a longtime area resident, died Tuesday, May 26, 2026, at Sharon Health Care Center in Sharon. Mr. Isham worked for the Tri-Wall Container Corp. in Wassaic, New York, for fifteen years and also worked as a self-employed private caretaker for over twenty-five years, caring for local estates in Shekomeko, Pine Plains and Ancramdale, New York, prior to his retirement.
Born Aug. 25, 1938, in St. George, Vermont, he was the son of the late Floyd Irving and Hazel (Thompson) Isham, Sr. Following his high school years, he enlisted in the United States Navy and served from 1958 until his honorable discharge in 1961. Mr. Isham also served in the Vermont National Guard. On Aug. 11, 1990, in Dover Plains, New York, he married Nancy L. Cross. Mrs. Isham died on July 8, 2005.
Mr. Isham was a life member of the Millerton American Legion Post # 178 in Millerton, and was a former member of the Amenia Fish & Game Club in Amenia. He served for eight years as president of the Dutchess County Federation of Fish & Game Clubs and also served on their legislative committee for a number of years. He was an avid hunter and fisherman and enjoyed gardening, watching the New York Mets and the Boston Red Sox on television and spent a great deal of time following the horses at OTB. Floyd will be deeply missed by his loving family and his many dear friends. Floyd’s family wishes to extend a heartfelt thank you to all the nurses, nursing assistants and staff at Sharon Health Care Center for the kind and respectful attention provided to Floyd while in their care.
Mr. Isham is survived by two children, Mary Kunda and Theodore Isham; three stepchildren, Candy Strong and her husband Bill, Brian Marshall and his wife Kathy and Tanya Mayhew; two grandchildren, Samantha Harrison and her husband Raymond and Cody Mayhew; one great grandchild, Harper Lee Harrison; several siblings and many nieces and nephews and friends. In addition to his wife and parents, he was also predeceased by three sisters, Lucille, Leonna and Roselyn.
Graveside services and burial will take place on Wednesday, June 3, 2026, at 11 a.m. at Ellsworth Cemetery, 25 Cemetery Road, Sharon with Standard Naval Honors. Pastor William Mayhew will officiate. Memorial contributions may be made to the Millerton American Legion Post # 178, 155 Route 44, Millerton, NY 12546. To send an online condolence to the family, flowers to the service or to plant a tree in Floyd’s honor, please visit www.conklinfuneralhome.com
Keep ReadingShow less
Pauline King Garfield
Lakeville Journal
Jun 03, 2026
EAST CANAAN — Pauline K. (King) Garfield, 94 of 77 South Canaan Rd. formerly of East Canaan, died Sunday May 24, 2026, at Geer Village. She was the wife of the late Duane Garfield who passed August 14, 2017. Pauline was born April 3, 1932 in North Canaan,in the former Geer Hospital. She was the daughter of the late Charles and Rose (Van Vlack) King.
Pauline spent her career at Becton Dickinson in Canaan, after being a stay-at-home mother for many years.She was employed at Becton Dickinson for 23 years. She enjoyed bus trips with her late husband Duane to the Casinos, spending time with her family watching the grandchildren grow up. Recently she made a comment to care givers that was “wait until I see that husband of mine for leaving me here, I am going to read him the riot act.” Over the years she enjoyed many crafts, but her favorite was crocheting gifts for everyone.
Pauline is survived by her daughter, Paula Ducharme and husband Tom of York, Pennsylvania, her son Michael Garfield and wife Joann of Winchester Center, Connecticut, her granddaughter Koren Garfield and her great grandchildren, Alyssa Jade, Addison Jacob and Brennden Leo of Colebrook, Connecticut.
Pauline is also survived by her sister, Althea Marshall and her husband Corky of North Canaan, Connecticut. She was predeceased by her brothers, Everett and Alan King.
A Celebration of Pauline’s life was held on Monday June 1, 2026, at 10:00 a.m. in the North Canaan Congregational Church 172 Lower Road East Canaan, CT 06024.Burial followed at Hillside Cemetery in East Canaan, CT. Memorial Donation can be sent to the North Canaan Volunteer Ambulance Corps P.O. Box 178 North Canaan, CT 06018. Arrangements are under the care of the Newkirk-Palmer Funeral Home 118 Main St. Canaan, CT 06018.
Keep ReadingShow less

Want more of our stories on Google? Click here to make us a Preferred Source.
loading